Good Bugs, Bad Bugs: Exploring the Link between Cancer and Vaginal Bacteria
Although one of the top 10 cancer types in the United States, a lot of people haven’t heard of endometrial cancer.
Although one of the top 10 cancer types in the United States, a lot of people haven’t heard of endometrial cancer. The endometrium is the lining of the uterus and endometrial cancer is projected to cause nearly 11,000 deaths in the United States in 2017 alone. We know little about what causes endometrial cancer, but scientists are hard at work to answer that question.
One such scientist is Melissa M. Herbst-Kralovetz, PhD, who leads the Women’s Health Microbiome Initiative. Dr. Herbst-Kralovetz and her team hope to figure out if endometrial cancer is affected by the vaginal microbiome — the bacteria that live in the vagina. While most of us are raised with the belief that germs are bad, only a fraction of a percent of microbes are harmful — while some are crucial to our health. Dr. Herbst-Kralovetz is working to find out which microbes are associated with good health and which types might be signs of endometrial cancer — knowledge that can help us develop treatments or prevention strategies.

Dr. Herbst-Kralovetz is an associate professor in the departments of Basic Medical Sciences and Obstetrics and Gynecology at the UA College of Medicine – Phoenix
What do we already know about the relationship between vaginal bacteria and endometrial cancer?
We know that an unbalanced vaginal microbiome contributes to significant health problems in women, including increased risk of acquiring sexually transmitted infections. Our hypothesis is that vaginal bacteria could travel up the reproductive tract, from the vagina into the uterus, where they might cause inflammation and damage to the epithelium, the tissues that line the inside of the reproductive organs. Although inflammation is a normal part of our immune response, there can be too much of a good thing and chronic inflammation causes tissue damage and DNA damage that ultimately drives cancer formation.
Both good and bad bacteria are critical in keeping our immune systems in balance by influencing things like inflammation and our susceptibility to infection. However, the role of vaginal bacteria in promoting inflammation and cancer, especially in the reproductive tract, is not well understood at this point.
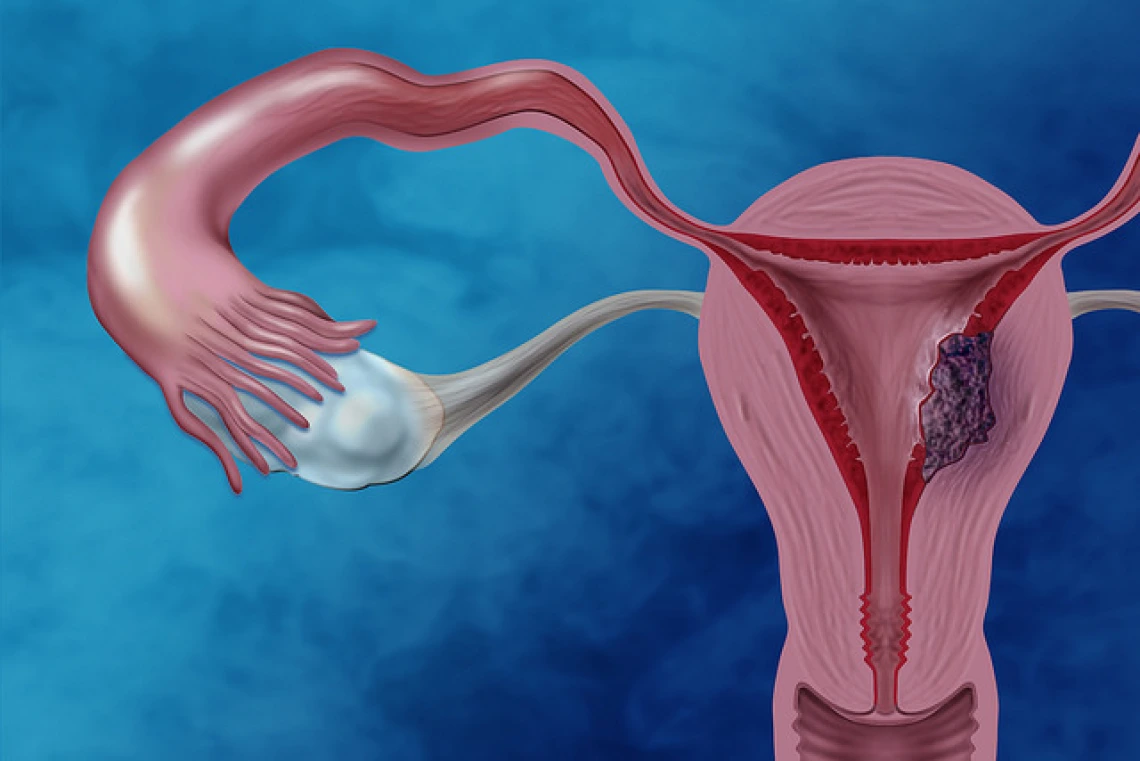
Dr. Herbst-Kralovetz research is meant to better understand the role of genital bacterial communities in the biology of inflammation and type I endometrial cancer as a means for risk reduction in women.
What questions do you hope to answer?
We are really at the ground floor with this research and investigating this hypothesis. We want to be able to address the relationship between vaginal bacteria and inflammation in women with endometrial cancer and without endometrial cancer, so we can explore the differences between the two groups. In addition, we want to identify bacterial species that are dominant during the early stages of cancer formation. Are these species influencing their environment at a cellular level? Can they cause cancer? Can they contribute to speeding along cancers that are starting to develop?
What comes first — bad bacteria or endometrial cancer? In other words, do you know if bad bacteria cause endometrial cancer, or if the cancer creates a hospitable environment for bad bacteria to flourish?
Great question! It is always difficult to figure out if the bacteria that live in our bodies cause disease, or if a disease creates an environment that favors certain bacterial species over others. Our Mary Kay Foundation grant will help us answer that question by allowing us to look at different stages (precancer and cancer). It’s the “chicken or the egg” concept. Do certain bacterial species predominate before a disease emerges, or does the disease emerge first, followed by an invasion of those bacterial species?
We are at an early stage, but if we know what bacteria might be acting as “drivers” or “passengers” in the formation of cancer, we can study them as individual species or as bacterial communities to understand how they alter their local microenvironment. Identifying drivers of cancer will allow us to use those microbial “signatures” as potential risk factors for the development of endometrial cancer.
Many people love the idea of buying “probiotics” — specially prepared bacteria that can colonize their bodies to promote better health. How far away do you think we are from evidence-based, commercially available probiotics to enhance women’s health?
Bacterial therapeutics are an exciting new area of research. However, more rigorous studies are needed before we can know if they’re effective in re-establishing a healthy balance of bacteria in the vagina. Additional research in this area is warranted.
About the Author
Melissa Herbst-Kralovetz, PhD, has a long-standing interest and background in infections that impact women’s health. Her lab is studying the lower female reproductive tract’s mucosal barrier, which plays an important role on the frontlines of the immune system by protecting the body from microbes. Specifically, Dr. Herbst-Kralovetz is interested in studying how vaginal bacteria interact with the reproductive mucosal barrier to set the stage for inflammation, tissue damage and ultimately cancer. She obtained her bachelor’s degree from Colorado Mesa University in Grand Junction and her doctorate from the University of Texas Medical Branch in Galveston. She is an associate professor in basic medical sciences and obstetrics & gynecology at the UA College of Medicine – Phoenix.

