Health Professions Programs to Expand, Diversify Workforce
Three new student programs aim to train the next generation of health care professionals and increase access to care across Arizona’s diverse communities.

Nurse-midwifery is one of three new University of Arizona Health Sciences programs seeking accreditation to expand access to care and address workforce shortages in critical health fields.
Approximately 3.2 million Arizonans – nearly 40% of the state’s population – live in an area with a current health care shortage, according to the Health Resources and Services Administration. The University of Arizona Health Sciences is working to alleviate that challenge by expanding the workforce in three health care fields: physical therapy, physician assistant and nurse-midwifery.
The Arizona Board of Regents recently approved the launch of the three new degree programs. Each of the new health professions programs will create an expanded pipeline of skilled providers to provide greater access to care for patients in Arizona’s diverse rural and urban communities. All three programs are independently seeking accreditation before they will be available for student enrollment.
Expanding access to care
Physician assistants (PAs) are licensed health care professionals who contribute to the primary care workforce by practicing medicine as part of a team. U.S. News and World Report ranks physician assistant No. 3 on its “100 Best Jobs” list.
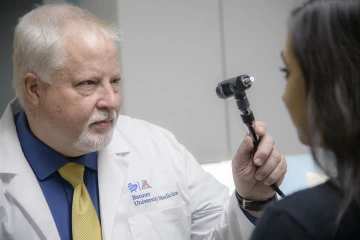
Kevin Lohenry, PhD, PA-C, says physician assistants are trusted, rigorously educated and trained health care professionals dedicated to expanding access to care and transforming health and wellness through patient-centered, team-based medical practice.
“PAs play an important role in helping increase access to care for patients,” said Kevin C. Lohenry, PhD, PA-C, University of Arizona Health Sciences assistant vice president for interprofessional education and director of the physician assistant program, which will be housed in the College of Medicine – Tucson.
Dr. Lohenry noted that physician assistants are increasingly being sought to address shortages of health care providers and the maldistribution of specialists in rural areas. In Arizona, almost 95% of the state’s physician assistant workforce practice in urban settings, according to the Center for Rural Health at the Mel and Enid Zuckerman College of Public Health.
The physician assistant program will be designed with an emphasis on rural primary care medicine. For example, medical Spanish will be a part of the curriculum to prepare students to serve Spanish-speaking patients throughout southern Arizona.
“As we build this program, we are excited to work with community partners in recruiting students from those areas of need, preparing them to practice patient-centered, team-based medicine, and supporting their eventual return to those communities as licensed PAs,” Dr. Lohenry said.
Training a new quality of professional
Unlike some health care professions, physical therapy is not facing a major workforce shortage at the national level. However, Arizona has fewer physical therapists per 10,000 residents than the national average. Many of the state’s physical therapists are located in urban areas, which does not meet the needs of Arizona’s rural communities.
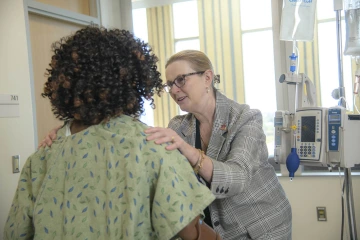
Christine Childers, PT, PhD, a geriatric clinical specialist, describes the evolving physical therapy field as one needing skilled therapists able to provide care specific to local populations. In southern Arizona, that includes meeting the needs of aging and Spanish-speaking populations, among others.
Additionally, Tucson’s population of individuals over the age of 65 is higher than the national average, resulting in additional clinical needs in cardiopulmonary, geriatrics and neurology. Currently, there is a lack of physical therapists with advanced certification in these areas, said Christine Childers, PT, PhD, founding director of the doctor of physical therapy program in the College of Medicine – Tucson.
“The goal of our program is to really tap into clinical affiliations and service learning, particularly in underserved communities, and get our students passionate and interested in serving in the communities that have a need for them,” Dr. Childers said. “We want students to be hands-on and helping people from day one.”
Service learning opportunities could include running an exercise program at an assisted living facility, working with after school programs or riding therapy for individuals with special needs. Other experiences could include taking vital signs at a mobile health clinic or any number of interprofessional education experiences with students in any of the five UArizona Health Sciences colleges.
“Our profession is transitioning to train a different genre of physical therapy professional,” Dr. Childers said. “Communication, emotional intelligence, cultural understanding and the ability to have empathy are skills that are equally as important as the scientific content.”
Creating a more diverse profession
When it comes to midwives, a common myth is they only provide care for home births.
“Certainly, that is something a nurse-midwife can do,” said Erin McMahon, EdD, CNM, FACNM, director of the nurse-midwifery program. “However, most certified nurse-midwives practice in the hospital setting.”
“We want students to be hands-on and helping people from day one.”Christine Childers, PT, PhD
A nurse-midwife can care for a person throughout their lifespan and address all aspects of their reproductive and sexual health, Dr. McMahon says. That can include cancer screenings, family planning, contraception, perimenopausal or menopausal care.
“It really covers a breadth of clinical needs,” Dr. McMahon said. “We do so by looking at the individual as a whole person and taking a holistic view of their health and wellness.”
The need for nurse-midwives is growing as the field of obstetrics and gynecology (OB-GYN) is seeing its workforce shrink. According to a 2017 report from the American College of Obstetricians and Gynecologists, nearly 1 in 3 OB-GYN doctors were aged 55 or older and nearing retirement. At the same time, younger doctors were trending away from general OB-GYN practice in favor of more specialized fields.

Erin McMahon, EdD, CNM, pictured in front of a birthing manikin in the Arizona Simulation Technology and Education Center, says there has been a push to increase the number of academic midwifery programs graduating more nurse-midwives.
Additionally, access to prenatal and obstetric services are decreasing in rural areas due to closures of obstetric units and rural and critical access hospitals. Several of Arizona’s counties have very few or even no obstetric providers. Nearly half of the women in some rural areas must travel for more than 30 minutes to receive maternity care.
Dr. McMahon believes the nurse-midwifery program, a new specialty within the College of Nursing doctor of nursing practice program, will address those issues. She hopes to recruit registered nurses from communities across the state who can then return to work in their communities as nurse-midwives.
“My goal is to establish a midwifery program that creates more nurse-midwives and develops a more diverse profession that is representative of the communities that we serve,” Dr. McMahon said.
Contact
Blair Willis
520-626-2101
bmw23@arizona.edu

