Implementing Rapid Care Guidelines for Pediatric Traumatic Brain Injury Patients Dramatically Improves Survival
An evaluation of emergency medicine guidelines showed proper care on the scene of a brain injury is critical to survival and ongoing brain health.

TUCSON, Ariz. — A University of Arizona Health Sciences-led study of prehospital care guidelines for emergency medical services providers treating traumatic brain injury (TBI) among children found deaths from severe TBI can be nearly eliminated if the guidelines are implemented by first responders.
The study, EPIC4Kids, is a follow-up to the larger all-ages Excellence in Prehospital Injury Care (EPIC) TBI study that showed that adjusted odds of survival doubled for severe head injury victims and tripled among those who were intubated using the guidelines.

Paramedics attend to a traumatic brain injury victim during a simulated crash at the City of Mesa Public Training Facility in May 2019. (Photo: Sun Belous, University of Arizona College of Medicine – Phoenix)
“For those kids with severe head injury, the adjusted odds of survival were 8.4 times higher after we started this,” said Dr. Gaither, who is an Arizona Emergency Medicine Research Center (AEMRC) member and Tucson Fire Department medical director.
Read how Glendale Fire paramedic Alex Matthews’ EPIC initiative training helped save her son’s life after they were involved in a traffic accident.

Joshua B. Gaither, MD (Photo: University of Arizona Health Sciences)
“Dr. Gaither’s work as part of the statewide AEMRC is a big milestone in the fight against traumatic brain injury,” said Samuel M. Keim, MD, professor and chair of the Department of Emergency Medicine, AEMRC director and a coauthor on the paper. “Because this work was with children, the future economic impact of improving outcomes is huge.”
According to the U.S. Centers for Disease Control and Prevention, the burden of TBIs includes about 2.9 million emergency department (ED) hospital visits in the United States a year and nearly 57,000 deaths. Among children, TBIs result in 837,000 ED visits and more than 2,500 deaths per year, making it the leading cause of pediatric death and disability.
EPIC4Kids study cases were drawn from Arizona State Trauma Registry data from the Arizona Department of Health Services and were scored based on severity – moderate, severe and critical. For the severe TBI group – the largest at 2,001 cases – the survival rate to hospital discharge increased to 100% after the implementation of the prehospital care guidelines.

Daniel W. Spaite, MD (Photo: University of Arizona Health Sciences)
The TBI guidelines, first introduced in 2007, focus on hypoxia, hypotension and hyperventilation – the “three H bombs” to avoid when treating head injury. All three cause a lack of oxygen or blood flow to the brain: the first involves low oxygen saturation in the blood; the second low blood pressure; and the third constriction of the arteries due to a carbon dioxide drop in the blood caused when an EMS provider squeezes a breathing bag on a patient faster than necessary.
To prevent hypoxia, EMS providers are taught to administer high-flow oxygen to patients right away. To prevent hypotension, they’re also taught to administer intravenous fluids quickly. To prevent hyperventilation, many EMS agencies now use special, flow-controlled breathing bags with a timing light as a visual cue for the proper rate. That rate, Dr. Gaither pointed out, varies from 20 squeezes per minute (every 3 seconds) for those age 14 and younger to 10 squeezes per minute (every 6 seconds) for older children and adults.
Daniel W. Spaite, MD, a professor and the Virginia Piper Distinguished Chair of Emergency Medicine and AEMRC associate director at the UArizona College of Medicine – Phoenix, said more than 11,000 Arizona paramedics and emergency medical technicians (EMTs) have been trained in the TBI treatment guidelines since 2012. This is important because less than a half-hour of prehospital treatment before hospital arrival is the most critical for TBI patient survival.

Simulated crash training crews with Alex Matthews (left), her son, Jamison (holding jaws-of-life device), and Glendale Fire paramedics. Alex and Jamison were in a motor vehicle accident in December 2012, where Alex used the EPIC-TBI prehospital care guidelines to help save the life of her son. (Photo: Sun Belous, University of Arizona College of Medicine – Phoenix)
“To think that, on average, the first 26 minutes of six-and-a-half days of medical care improved adjusted odds of survival by more than 700% in severe head trauma – it shows how quickly the neuron, the brain cell, dies. If you don’t do it right early – if you deliver a dead brain cell to the hospital– it doesn’t matter how good the neurosurgeon is, they’re not going to get it back. So it’s really remarkable,” said Dr. Spaite, who is the medical director for the City of Mesa Fire and Medical Department and co-principal investigator on the EPIC and EPIC4Kids studies.
Dr. Gaither underscored a need for regular reviews of head injury cases with first responders by EMS medical directors to reinforce that the guidelines, which cost little or nothing to implement, are followed.
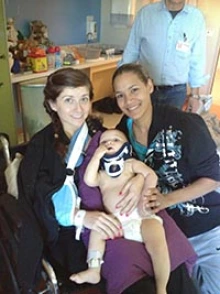
Glendale, Arizona, paramedic Alex Matthews (right), her son and her then-sister-in-law Amy Rodriguez (left) were severely injured after a crash in December 2012 at a Peoria intersection. (Photo: University of Arizona Department of Emergency Medicine)
“There’s absolutely no reason why any EMT or paramedic couldn’t implement these standards of care,” he said. “But getting our providers to focus on these truly critical interventions requires weekly feedback to ensure they’re implementing these strategies. That type of quality-improvement initiative is what will make a difference in communities across the country.”
If the EPIC-TBI treatment guidelines were implemented across the U.S., thousands of brain injury deaths among children could be prevented, Dr. Spaite said. To that end, he and Dr. Gaither are planning a nationwide study on TBIs to leverage the findings of the EPIC and EPIC4Kids studies.
Other authors on the EPIC4Kids paper include: Bentley J. Bobrow, MD; Samuel M. Keim, MD; Bruce J. Barnhart, RN, MSN; Vatsal Chikani, MPH; Duane Sherrill, PhD; Kurt R. Denninghoff, MD; Terry Mullins, MPH; P. David Adelson, MD; Amber D. Rice, MD; Chad Viscusi, MD, and Chengcheng Hu, PhD.
The EPIC4Kids study was supported by the National Institute of Neurological Disorders and Stroke, a unit of the National Institutes of Health (3R01NS071049-S1).
# # #
NOTE: Images and video available here – https://arizona.box.com/s/rx1eotm1xvjjxrl5thu7eo13y7relche
About the University of Arizona College of Medicine – Tucson
The University of Arizona College of Medicine – Tucson is shaping the future of medicine through state-of-the-art medical education programs, groundbreaking research and advancements in patient care in Arizona and beyond. Founded in 1967, the college boasts more than 50 years of innovation, ranking among the top medical schools in the nation for research and primary care. Through the university's partnership with Banner Health, one of the largest nonprofit health care systems in the country, the college is leading the way in academic medicine. For more information, visit medicine.arizona.edu (Follow us: Facebook | Twitter | Instagram | LinkedIn).
About the UArizona College of Medicine – Phoenix
Founded in 2007, the University of Arizona College of Medicine – Phoenix inspires and trains exemplary physicians, scientists and leaders to optimize health and health care in Arizona and beyond. By cultivating collaborative research locally and globally, the college accelerates discovery in a number of critical areas — including cancer, stroke, traumatic brain injury and cardiovascular disease. Championed as a student-centric campus, the college has graduated 500 physicians, all of whom received exceptional training from nine clinical partners and 1,800 diverse faculty members. As the anchor to the Phoenix Biomedical Campus, which is projected to have an economic impact of $3.1 billion by 2025, the college prides itself on engaging with the community, fostering education, inclusion, access and advocacy. For more information, please visit phoenixmed.arizona.edu (Follow us: Facebook | Twitter | YouTube | LinkedIn | Instagram).
About the University of Arizona Health Sciences
The University of Arizona Health Sciences is the statewide leader in biomedical research and health professions training. UArizona Health Sciences includes the Colleges of Medicine (Tucson and Phoenix), Nursing, Pharmacy, and the Mel and Enid Zuckerman College of Public Health, with main campus locations in Tucson and the Phoenix Biomedical Campus in downtown Phoenix. From these vantage points, Health Sciences reaches across the state of Arizona, the greater Southwest and around the world to provide next-generation education, research and outreach. A major economic engine, Health Sciences employs nearly 5,000 people, has approximately 4,000 students and 900 faculty members, and garners $200 million in research grants and contracts annually. For more information: uahs.arizona.edu (Follow us: Facebook | Twitter | YouTube | LinkedIn | Instagram).

