Arizona AHEC: Filling a need for health care professionals
The Arizona Area Health Education Center Program and six Regional Centers aim to enhance access to quality health care in the state.

The Arizona Area Health Education Centers Program seeks to improve the supply and distribution of health care professionals, particularly primary and preventive care, in Arizona’s rural and medically underserved communities.
Access to health care is a right, not a privilege, yet millions of Americans lack the ability to obtain health care services that prevent, diagnosis, and treat diseases and address the social determinants that impact health.
Almost 100 million Americans live in a designated Primary Care Health Professional Shortage Area, defined by the Health Resources and Services Administration as areas and populations experiencing a shortage of primary care physicians relative to the population. In Arizona alone, more than 3.3 million people live in Health Professionals Shortage Areas.

As a medical resident, Judith Hunt, MD, did rotations through the Arizona Area Health Education Center program in Nogales, Arizona. Now, she gives back to Arizona AHEC by teaching medical students and residents about rural health care in Payson, Arizona.
But in one 12-month period, more than 1,500 health profession trainees – future physicians, nurses, pharmacists, dentists, phlebotomists, physician assistants, physical therapists, public health professionals and more – participated in community-based experiential training thanks to a long-standing University of Arizona Health Sciences program. Since 1984, the Arizona Area Health Education Centers Program has served the state through health professions workforce training, recruitment and retention in rural and medically underserved communities.
“My rural medical experiences have been vital in preparing me to be a competent full-spectrum family medicine physician,” said Amanda McKeith, MD, a resident in the UArizona College of Medicine – Tucson’s Department of Family and Community Medicine. “When your community has limited access to resources and specialists, patients depend on family medicine doctors to provide them with the care they need. My rural rotations ensure I develop these necessary skills. Where else can you learn to deliver a baby, perform a post-partum tubal [ligation], admit a patient to the ICU and perform a shoulder reduction – all in one day?”
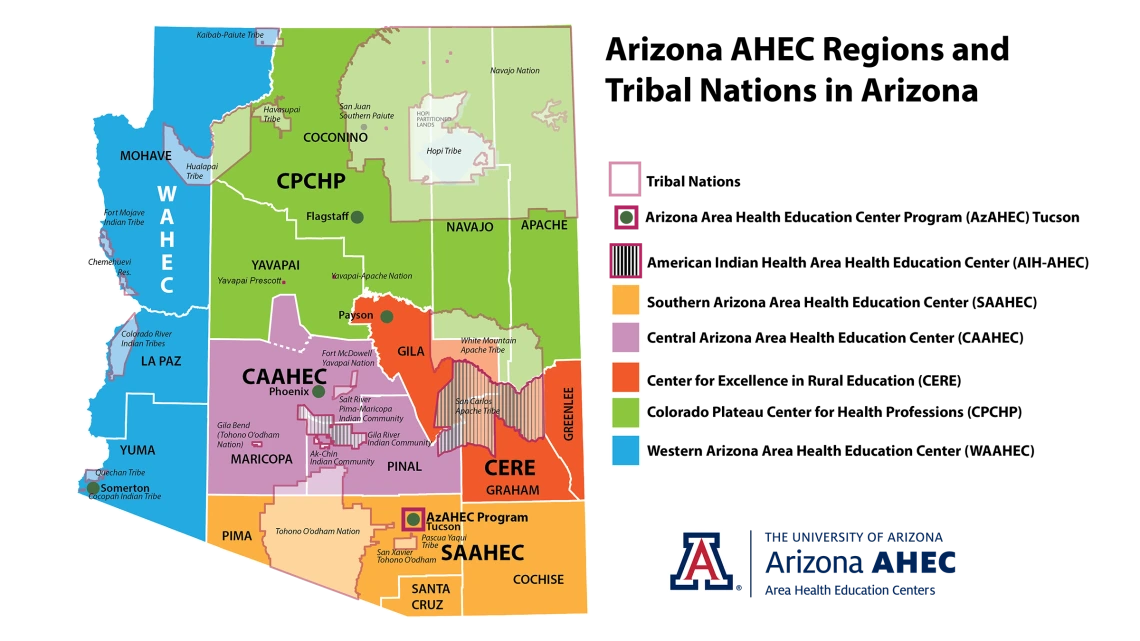
Six AzAHEC Regional Centers enhance access to quality health care, particularly primary and preventive care, by improving the supply and distribution of health care professionals through academic-community educational partnerships in rural and urban medically underserved areas as part of the Federal Area Health Education Program.
A history of developing a diverse health care workforce

Students from the Mel and Enid Zuckerman College of Public Health participate in a service-learning event at Tierra Anita Community Garden in Tucson. The garden, a partnership between the Barrio Anita neighborhood and the Primavera Foundation, increases access to fresh, healthy foods while strengthening community bonds.
The explosive population growth seen during the “baby boom” from 1946 to 1964 added 76 million people to the U.S. population. Congress, concerned there would not be enough health professionals to care of the growing population, authorized the Area Health Education Centers program in 1971 to recruit, train and retain a health professions workforce committed to rural underserved populations.
Fifty years later, the need continues. There are currently 56 AHEC Programs and 235 Regional Centers in the U.S., including six in Arizona. In the last fiscal year, the AzAHEC Program and the AzAHEC Regional Centers provided 12% of the community-based, health profession training rotations reported by the 56 AHEC Programs in the U.S.
“Interprofessional, community-based experiential training rotations are vital to improving access to health care for all Arizona residents, especially those living in rural and urban underserved areas,” said Daniel Derksen, MD, senior advisor and principal investigator of the AzAHEC Program and University of Arizona Health Sciences associate vice president for health equity, outreach and interprofessional activities. “The first Arizona AHEC Regional Center opened in Nogales in 1984. By 1989, we were serving all 15 Arizona counties through five Regional Centers. Last year, we expanded to six with the addition of the American Indian Health AHEC Regional Center.”
Training culturally appropriate health care providers
The American Indian Health AHEC Regional Center, in collaboration with the San Carlos Apache Healthcare Corporation and Gila River Health Care, are implementing education and training to improve the supply and distribution of health care professionals in tribal communities. They work with many of the 22 federally recognized tribes in Arizona.

The Rural Health Professions Program prepares students from the University of Arizona, Arizona State University and Northern Arizona University to practice in rural communities, where access to specialists is often unavailable.
“Tribes in Arizona experience a serious shortage of health care professionals compared to other regions in the state,” said Leila Barraza, JD, MPH, director of the AzAHEC Program and associate professor of community, environment and policy in the Mel and Enid Zuckerman College of Public Health. “The American Indian Health Regional Center can begin to alleviate some of these shortages by working closely with our tribal health systems and enhancing their current workforce strategies.”
On July 1, 2022, the American Indian Health AHEC Regional Center joined five existing AHEC Regional Centers in Arizona: the Central Arizona AHEC; the Colorado Plateau Center for Health Professions; the Southern Arizona AHEC; the Center for Excellence in Rural Education; and the Western Arizona AHEC.
“At my rural health clinical site, I had a wonderful experience. My preceptor was extremely knowledgeable and a great teacher,” said Allison “Kate” Macias, RN, who works at the Chandler Regional Medical Center and recently graduated with a Doctor of Nursing Practice – Family Nurse Practitioner degree from Arizona State University. “I thoroughly enjoyed caring for patients in this rural, Federally Qualified Health Center setting. The population is unique and requires many resources and holistic care. My experience at this clinical site reaffirmed by passion for rural and underserved patients and gave me great experience and knowledge in caring for them.”
Each year, the AzAHEC Program and Regional Centers partner with the nine Rural Health Professions Programs based in Arizona’s three public universities – the University of Arizona, Arizona State University and Northern Arizona University – professional organizations and communities to provide a variety of training and educational events. During fiscal year 2021-2022:
- 1,531 students and residents representing 40 universities and residency programs participated in 3,022 field experiences around Arizona, with 75% indicating the rotation increased their likelihood of practicing in a rural or medically underserved area;
- 609 students from UArizona, ASU and NAU received 1,158 training experiences through the nine Rural Health Professions Programs;
- Nearly 4,500 health professionals attended 136 continuing education events, with 90% indicating they were likely or very likely to implement the materials into their practice;
- 2,749 local community members attended health education activities and events;
- 1,376 K-12 students participated in health career programs, with more than 97% of high school students reporting that they were very interested in pursuing a health career;
- 13 undergraduate and 92 graduate students received advanced community-based experiences through the AzAHEC Scholars Program.
“I am proud to participate in this important scholar program. As a future nurse practitioner, I know that this opportunity will benefit my practice,” said AzAHEC Scholar Marian Brock-Anderson, MSN, RN, who is working as a clinical instructor for the UArizona College of Nursing while pursuing a Doctor of Nursing Practice – Family Nurse Practitioner degree at ASU. “Rural and underserved communities benefit directly from groups that work as partners to develop and implement programs to serve their unique needs.”
Our Experts
Leila Barraza, JD, MPH
Director, Arizona Area Health Education Center Program
Associate Professor, Mel and Enid Zuckerman College of Public Health
Dan Derksen, MD
Associate Vice President, Health Equity, Outreach and Interprofessional Activities, UArizona Health Sciences
Senior Advisor, Arizona Area Health Education Center Program
Director, Center for Rural Health
Professor, Mel and Enid Zuckerman College of Public Health
Professor, Department of Family and Community Medicine, College of Medicine – Tucson
Walter H. Pearce Endowed Chair in Rural Health
Contact
Stacy Pigott
Health Sciences Office of Communications
520-539-4152
spigott@arizona.edu

